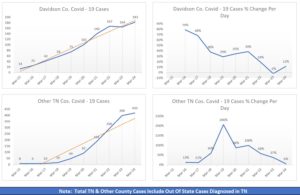
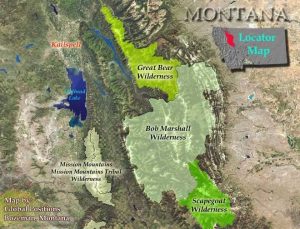
Notes From The Road | The Bob Marshall Wilderness Complex consists of three wilderness areas in Montana totaling over 1.5 million acres. Located in the northern Rocky Mountains along the Continental Divide, the region is as primitive as any found in the United States outside of Alaska. It’s also diverse, encompassing the dry and open Rocky Mountain Front Range on the east, and the lush and heavily timbered Swan Range and Flathead Range on the west.
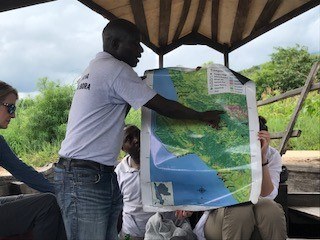
As a result, it is the most ecologically complete mountain wilderness in the country. Every species of mammal indigenous to the Northern Rockies still lives in this area and adjacent Glacier National Park, except bison and woodland caribou. Huge herds of elk, bighorn sheep, and mountain goat roam the region’s rugged peaks, big river valleys, large meadows, and vast coniferous forests. The Complex is prime Grizzly bear habitat; the population density is higher there than anywhere else in the lower 48 states.
Tracy and I had the opportunity to spend nine days in this vast national treasure last month, confirming for me—yet again—the inestimable value of our country’s wild lands.
We had no connectivity while we were there, so I jotted down notes at night and shared them (and pictures) when we returned.
“Man’s heart, away from nature, becomes hard; [the Lakota] knew that a lack of respect for growing, living things soon led to lack of respect for humans too.”
– Luther Standing Bear, Lakota Chief
Day 1. Tracy and I showed up at Lazy P Ranch on edge of the Bob Marshall Wilderness (the 1.5-million-acre crown jewel of the American wilderness system) for all-participant dinner, followed by an enlightening discussion of conservation of public lands, and critical multi-generational role of organizations such as The Wilderness Society and The Nature Conservancy. Conversation quickly turned to those special, local individuals who actually make possible the rich experiences and journeys into pure, untouched nature, like the ranges and basins we will explore over the next 8 days. Dusty, Danelle, Gene and others have led the way. For the first time in 29 years (transplant patients, political constituents, business), I turn off ALL electronic contact. Step one to achieve connection to nature and real world around us.

Day 2. Met Pat and Nickel early in this morning. They are strong, experienced, and loyal. They can be trusted through easy and tough times. They are the pros. They are the two horses for Tracy and me for the next seven days. And we met the 13 huge pack mules who will dependably carry our food, tents, supplies and everything else for the next 8 days. We set off on Route Creek Pass headed to Wrong Creek camp (13 miles). We soon saw our first bear. Alternating between woods and open spaces built our anticipation for the big climbs ahead. The power and grace of the mules working in harmony was the most amazing! We are beginning to taste the wildness and feel the grandeur. A little bit behind our motivation for the journey is caught in the words of American naturalist John Burroughs, “I go to nature to be soothed and healed, and to have my senses put in order.” What a rich inheritance from past generations are these vast and spectacular publicly (you and me and all of us) owned lands.
Day 3. Today we get closer in touch with the wild spaces. Big hike and a little fishing; Tracy’s hat becomes more colorful as we traverse meadows, scale hillsides and descend to and through the crystal clear creeks. Fresh drinking water from the creeks. Sore just a bit. Long rides on horseback use tiny muscles all over the body (little ones that had no names in medical school but still ache when taken to their limits!). Mules and horses were “belled” and allowed to roam freely for forage and grazing when not working! The clanging bells in the distance become a familiar, soothing melody.

Wilderness. Untouched by roads, or structures – just hiking and packing, with no evidence of humans. The unspoiled nature is allowed to evolve, as it has for millions and millions of years. Now the primitiveness is settling in, and it is calming, centering, and healthy. Brings to mind what is behind Thoreau’s powerful words, “In wildness is the preservation of the world.”
Day 4. Out of camp at 9:30 after packing tents, first mountain goats observed high up to the left along the Chinese Wall (Swep said one was three–legged, which kept us looking). The Chinese Wall is a thousand-foot high scarp of limestone that stretches for a dozen miles—a dramatic manifestation of the Continental Divide that we paralleled on our journey. The Wall is the rocky playground for these agile goats. Leisurely lunch on Pendleton blanket Tracy wisely brought and tied daily to her saddle with rain gear, as we marveled at the long, continuous, nose to tail, pack of muscular mules calmly yet determinedly marching by us.
Further north, we come to the limestone and red shale North Wall, about 10 miles long and seemingly even more primitive. Our trail followed the foot of this towering rampart, its starkness contrasting to the wildflowers and berries and grasses in meadows at the base of the towering cliff. I really need to learn the names and more about these berries, and flowers, and their lifecycles.
Highlight for Tracy and me: after a short hike, bravely swimming (only about 10 strokes because so cold!) in gorgeous, high mountain lake, Lake Levale, set against the backdrop of the rugged North Wall (seems like huge human faces carved into its side) and blue sky studded with journeying cumulus clouds. Arctic grayling fish were surfacing continuously, making ripples across the otherwise smooth turquoise waters. The spiritual experience is beginning to settle in. You see why the wilderness is known as Nature’s Cathedral.
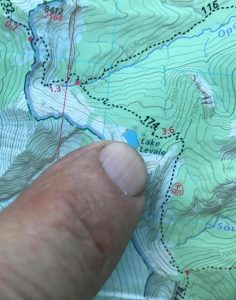
Tent positioned a little too much downhill last night which continued to ball up each of us at the foot of the tent all night. Hard to scoot uphill every hour in a sleeping bag. Will be more careful in choosing a flatter spot – even a few degrees matters!
It’s been four days without internet, TV, smartphone. The inner self is beginning to merge with the outer without all the clutter of oncoming! As Ralph Waldo Emerson wrote: “The lover of nature is he whose inward and outward senses are still truly adjusted to each other.” We, now 4 days in the wilderness, begin to feel this adjustment. We need to make sure this environment of pure nature is preserved for generations to come.
Day 5. We are a long, long way from civilization! Solitude and appreciation and humility as we connect with our horses and full blown nature. Today we pass from deep gladed forests to open, steep avalanche slopes of rocks devoid of trees. We feel the raw power of nature in these contrasts. Most intense feat thus far – traversing Switchback Pass! Actually we just hung on to their mane leaning as far forward as possible as our powerful horses boldly climbed the steepest and most rugged of the switchbacks, up the sheer mountain along the North Wall Trail. Talk about humbling!
As we were forewarned, today was the day we ran into a patch of bees, the horses anxiously reacting as you might expect with swarms of stinging bees, but all anticipated and taken in stride. Just keep moving when the going gets challenging! Swam in Trilobite lake which felt good and cleansing, with a belled mule joining for a drink at the edge, looking on nonchalantly. Lots of berries along the trail today. Tracy and I share together the reverence for these awe-inspiring wild places. “Look deep into nature, and then you will understand everything better” explained Albert Einstein.

Day 6. “Breakfast” – every morning at 7 am, the familiar piercing shout seems to come just a little too soon and way too commanding. We must be totally packed and ready to go before that call. But after breakfast we have the easy part, take down the tents, while the crew pack, tie, lift and secure two heavy, heavy (as much as 200 pounds each) manties to every mule. Performed, it seemed, like a smooth surgical procedure – though so much more muscular. Not to mix metaphors, but the whole morning prep for departure of 16 horses and 13 mules is like at grand symphony in the wilderness.
I know tying and knots — but only surgical knots. Nothing about real knots. The trip was full of “learnings” and today was knot tying. As others climbed peaks Tracy and I found solitude. Amidst breathtaking mountains and clear clean air. No roads, no devices. Just embracing nature and sounds of breezes, bumble bees, and butterflies (really). Relaxing, calming, centering. Clutter falls away. Thoughts seem a little clearer. “We need the tonic of wilderness,” reflected Thoreau.
We should actively protect this connection to nature so our great grandchildren (and theirs) can experience. These public lands are ours and we are their custodian. Once wilderness taken away it can never be regained. It is lost forever. Too many words from Washington today suggest that these public lands are at risk. We need to be smarter.
Day 7. Ten miles total ride today riding to Basin Creek. Half way we came to Gooseberry cabin, literally the only man-made structure we have seen all week. We are immersed in pure, unadulterated wilderness. No manifestations of man, road or structure anywhere, and we leave it just that way. Tracy and I found a huge shade tree for our packed lunch that we carried each day in our horn bags (along with a lot of water) and we both nap lazily. We had been advised to bring the best rain gear we could buy, but so far all sun. But at around 8 pm the clouds darkened. The saddles were covered and we prepared for rain. Off to our tents for cover, pulling all our gear inside for protection, where for the next hour we were enchanted and entertained by a huge thunderstorm with repeating flashes of lightening, heavy, recurrent rolls of thunder all around us, wind lifting our tent flies, and rain spattering against our tents. The raw power of nature speaking. Then suddenly all silent. Perfectly quiet.

Day 8. Sun River Pass Trail. Trace and I hang around camp today as others off to fish and hike. Carson had given me the best pointers on chopping wood efficiently yesterday and safely (he started by saying my sandals were not safe, my pack boots much safer), so after everyone was out of camp, I chop as much wood as I could, not for a campfire because it was too dry for that, but just because I could. Something in nature just wants you be a part. As Churchill said, “Nature will not be admired by proxy.” I stack the wood neatly (and vertically to make it seem like a lot) as I go to measure my progress. Tracy chops so much better than me! Off for a hike up the trail we came in on and then through a flowing meadow to a split in the crystal clear creek for lunch – and taking the opportunity to lie on the bank on our backs to rinse our hair (without having to get all the way in – cold water!).
A huge, fire in 1988 left miles and miles of the landscape with an otherworldly feel – only the charred trunks of the lodgepole pine were left standing, void of all branches or greenery. Undergrowth of aspen and pine are just beginning.
Day 9. Today is our last day on the trail – 14 miles. Billed as an “easy 14” but it seems a bit tougher, maybe because we “smelled the barn.” In and out of the woods, meadows, valleys, and hills, all is gorgeous. No grizzly bears (yes big tracks!) or mountain lions, but mule deer are common. Even Luke, who is 14, said on a scale of 0-15, that his aches were a “4”. Curiously but nonchalantly, he remarked agreed, thinking I was about a 7”. We pull up at a coral, the terminus of our journey. Beef jerky, crackers, cold drinks awaited, as we loaded our saddles in trailers. How could it be over? We are just now becoming one with nature. We are filled with more understanding and more humility and more fulfillment.
Einstein had it right: “Look deep into nature and you will understand everything.”